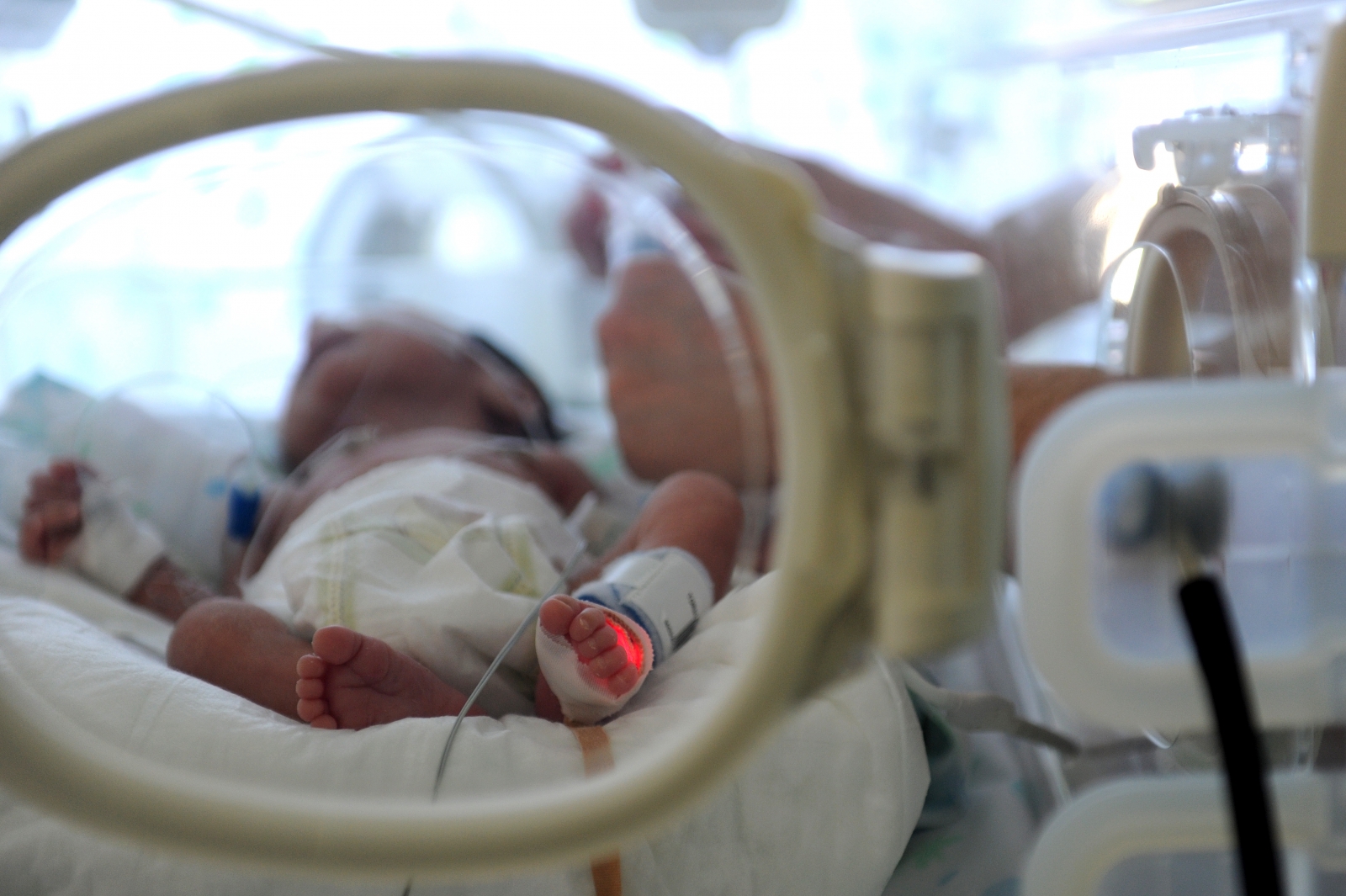
The implication was that the maternal body was inconsequential, a mere container The French physician Alexandre Lion found success with a similar model, creating an incubator that included a thermostat and heating system intended to function without the need for nurses. Although it had a glass cover, the Rotch-Putnam incubator – tellingly called a ‘brooder’ – was shrouded in black cloth, and included built-in scales to weigh the baby without removing it. The American paediatrician Thomas Rotch believed that his device should mimic the womb by creating ‘a condition of darkness, silence, and warmth’. The hermetic-womb model became particularly popular following the launch of the Rotch-Putnam incubator at the World’s Columbian Exposition in Chicago in 1893. Incubators became something of a fairground attraction, generating enthusiastic crowds at the various world fairs and expositions that sprung up in the Victorian era. His incubator was glass-topped and placed at the end of the mother’s bed in the belief that keeping the infant within her view would help with attachment.Įven so, the press and public in Europe and the United States relished the idea of using the technology to replace rather than enhance maternal connection. The French physician Pierre Budin emphasised the connection between mother, premature baby and nurse.
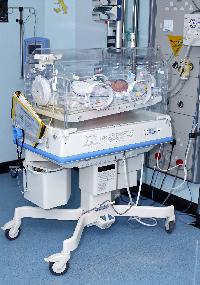
Other obstetricians favoured a more open model that brought together maternal and medical care. These attempts to recreate the womb were accompanied by early obstetricians’ concern that mothers themselves, with their unsanitary practices, irresponsible behaviour and anxious fussing, might pose a danger to their infants – a danger that could be curbed by placing the uterus-incubator firmly in the doctors’ hands.
#Baby incubator full
In Germany in the 1880s, the gynaecologist Franz Winckel trialled a ‘permanent water bath’ at Dresden Royal Maternity Hospital, in which the baby would be suspended in a pool of warm water, just as it would have stayed in the warm amniotic fluid had its birth gone to full term. Tarnier and his protégé Alphonse Pinard believed that the incubator should remain a closed system, self-contained and impenetrable to light, and ‘analogous to the womb’. Many doctors and scientists cast the early incubator as an environment that was safer than a ‘real’ uterus, as the medical historian Jeffrey Baker writes in The Machine in the Nursery (1996). This confidence gave rise to a tension that would permeate much of the subsequent scientific and popular literature: was the incubator intended to enhance connection between the premature infant and its carers – to act as a bridge to the mother? Or was it intended to replace her? Tarnier felt that he was on the cusp of enabling premature babies to survive from a significantly earlier point in gestation. Yet his invention was significant, not so much for its novelty or impact, but because it framed the premature baby as an entity distinct from full-term infants. Tarnier’s incubator probably drew on these earlier designs, and was reasonably modest in its ambitions: a couveuse would likely have been used for babies born no more than a week premature.

In Europe, those caring for new babies often used hot-water bottles and blankets after the birth where available, they also deployed higher-tech interventions, such as metal warming tubs (‘ warmwännen’), heated by a jacket of warm water. The French obstetrician Stéphane Tarnier was so impressed by the heating devices that the zookeeper used to hatch eggs, he asked him to build a similar box (a ‘ couveuse’) for what were then called ‘weaklings’ or premature and low birth-weight infants at the maternity hospital. According to the apocryphal story, the birth of the incubator took place in the Paris Zoo in the late 1870s. I spent the first few days of my life in an incubator but, until quite recently, I gave the technology relatively little thought.
